There's nothing like becoming a father
The problem is, it’s not always easy. In 60% of cases, a male factor, such as a low sperm or semen count, contributes to a couples’ infertility. Maze specializes in Reproductive Health treatment for patients in Westchester, New York City NYC, Connecticut, and New Jersey. We’re here for you and we can help.
Least invasive, Most Effective Treatment Options

Let's start with the science:
Roughly 60% of the time, male infertility is the primary reason why couples can’t have children14. Fertility, however, is a broad and complex subject. So diagnosing and treating its causes takes exceptional skill and, in many cases, specialized training. Few facilities have the technical expertise to treat infertility effectively, which is one component that sets Maze Men’s Sexual and Reproductive Health apart from other providers.
Michael A. Werner, MD, Maze’s founder, is eminently well-qualified. A board-certified urologist and microsurgeon, Doctor Werner has written extensively and lectured widely on male infertility and sexual dysfunction. His knowledge of advanced techniques is unsurpassed. For example, he routinely performs varicocelectomies, a highly successful way to reverse male infertility — that is also minimally invasive.
Doctor Werner is the only physician in the U.S. offering Extended Sperm Search & Microfreeze (ESSM), which has found sperm in 44% of men who were diagnosed with azoospermia, or no sperm in the ejaculate. Furthermore, he has also pioneered a groundbreaking procedure that combines two existing techniques that both diagnoses the presence of sperm and procures it in one minimally invasive procedure.
Which brings us to common sense...
At Maze, finding the best possible treatment for you means choosing procedures that are the least invasive, the most cost-effective and, above all, the best suited to your individual needs.
We will pursue multiple paths of inquiry. Most patients come in with a wife or partner, so if there’s any possibility that her infertility is at issue, we’ll suggest that she pursue a parallel exploration with outside experts whom we respect. (Maze doesn’t treat female infertility directly). By coordinating our efforts with those experts, we’ll find a treatment that makes the best use of your resources.
Reproductive Health Issues
Male Infertility
Male infertility is a broad and complex area, so the information presented here should be seen as a general introduction. That said, you may be unaware that, in 60% of cases, a male factor contributes to a couples’ infertility14. That’s why it makes sense to evaluate the man’s role as well as the woman’s in these cases, and to know that there are a variety of male infertility treatments to help a couple reach their goals.
No Sperm/Azoospermia
Azoospermia is the term that’s used when there is virtually no sperm count in the ejaculate. Even if this is the case, the surprising reality is that sperm may still be produced but not delivered to the semen, or that interventions may help the man produce sperm. In those cases where, after intervention, there is still no sperm in the ejaculate, there may be a possibility of harvesting small amounts of sperm, which have been produced in the testes as a result of the interventions. These sperm may be used in in vitro fertilization (IVF) or intracytoplasmic sperm insertion (ICSI).
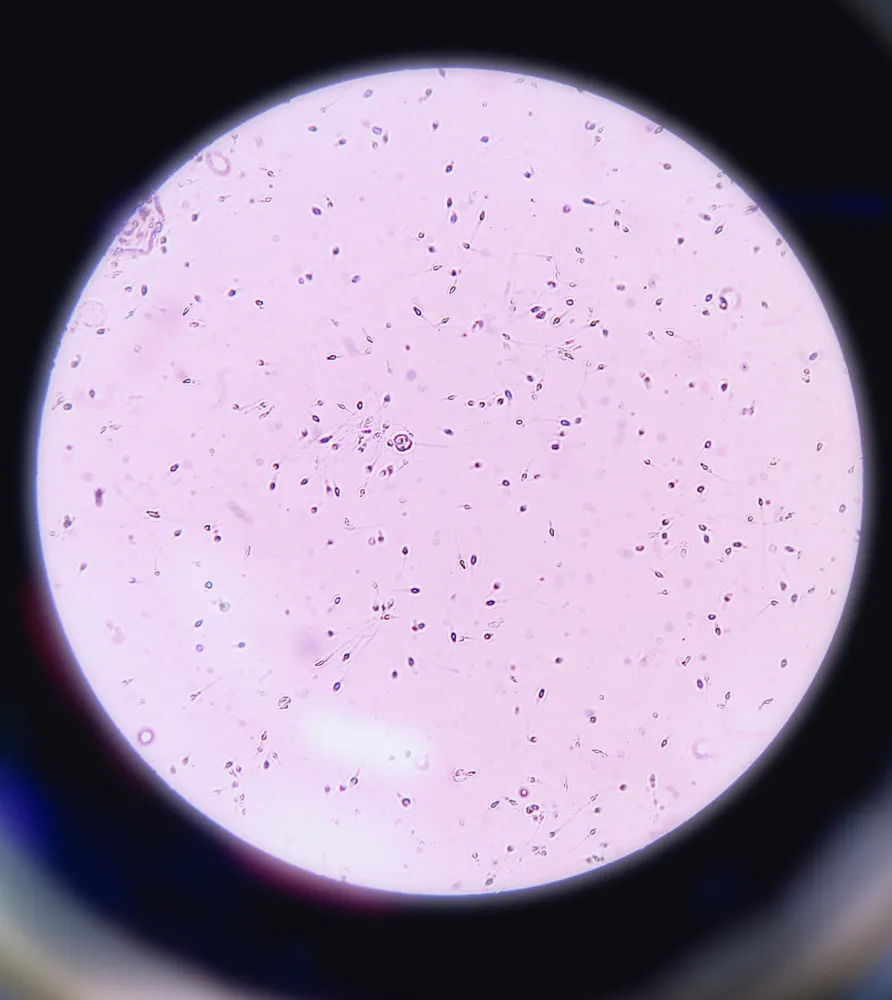
Semen Analysis
Extended Sperm Search & Microfreeze (ESSM)
In 44% of azoospermic men, there will be a small number of sperm that exists in the ejaculate but can’t be detected in a standard semen analysis. ESSM is a revolutionary, new procedure, performed exclusively at Maze in the US, that effectively finds and freezes sperm.
Sperm Mapping
Sperm mapping, or Testes mapping, is a procedure done on the testes to determine if there are sperm producing areas in the testes. This test is useful because the testes are “heterogeneous” meaning that different areas of the testes have different patterns of sperm production. Thus, although a majority of the areas of your testes may produce no sperm, there may be some harder-to-find areas that do. The importance of sperm mapping is it can tell us if there are sperm producing areas in the testes, and where they are.
Sperm Extraction Procedure
We have recently pioneered the use of combining the diagnostic value of the Sperm Mapping procedure with the therapeutic value of collecting sperm at the same time using Extended Sperm Search & Microfreeze (ESSM). We have termed this Grid Needle Sperm Extraction and Microfreeze or GN-SEM.
Varicocelectomy
If you’re familiar with “varicose veins” in the legs, you will understand varicoceles as the same condition, a dilated (enlarged) group of veins, but in the scrotum. The dilated veins are filled with excess blood. Studies show, with an unusual degree of unanimity, that there is one best way to repair a varicocele: the microscopic sub-inguinal varicocelectomy with ultrasound guidance.
Epididymal Obstruction
There is a crescent-shaped duct within the scrotum that collects sperm from the seminiferous tubules, called the epididymis. While sperm are passing through the epididymis, they mature and gain movement. In some men, the epididymis becomes blocked, preventing sperm from entering the vas deferens and getting into the ejaculate. An epididymal obstruction does not mean you have untreatable infertility. There are a number of options available to patients suffering from the blockage.
Sperm Banking
Whatever your reason for cryobanking, Maze offers a full line of services to collect, freeze and store sperm. To ensure the future viability of your sperm, we first perform a thorough semen analysis prior to banking. A cryopreservative is added, and the specimen is divided into individual tubes, each labeled with multiple unique identifiers.
Vasectomy
In a no-needle, no-scalpel vasectomy, it is the anesthesia that is different. The surgeon uses a device similar to a strong spray gun that allows the anesthesia to be given through the skin, which then infiltrates the tissues underneath. With a conventional vasectomy, numbing medication is injected into the spermatic cord and all of its structures.
THERE'S NOTHING LIKE BECOMING A FATHER
Last updated: November 2021