Epididymal Obstruction
The epididymis is a long coiled tube located on the back of the testis; it collects and stores sperm. An epididymal blockage or obstruction can form, preventing sperm from getting into the ejaculate. Maze specializes in Epididymal Obstruction for patients in Westchester, New York City NYC, Connecticut, and New Jersey. Fortunately, it’s completely treatable and we can help.
Maze’s Unique Approach to Epididymal Obstruction
At Maze Men’s Health, led by Michael A. Werner, MD, we specialize in diagnosing and treating epididymal obstruction—a common but often overlooked cause of male infertility. This condition occurs when sperm are produced normally in the testicles but are blocked from entering the ejaculate due to a blockage in the epididymis, the delicate coiled tube behind each testis.
Our approach begins with a detailed diagnostic evaluation to determine whether the issue is one of production or delivery, followed by a personalized treatment plan that can include microsurgical reconstruction (vasoepididymostomy) or minimally invasive sperm retrieval (MESA or testicular biopsy). At Maze, we help men across Westchester, New York City (NYC), Connecticut, and New Jersey restore fertility and regain control of their reproductive health through science-based, compassionate care.
Understanding the Epididymis and Its Role in Fertility
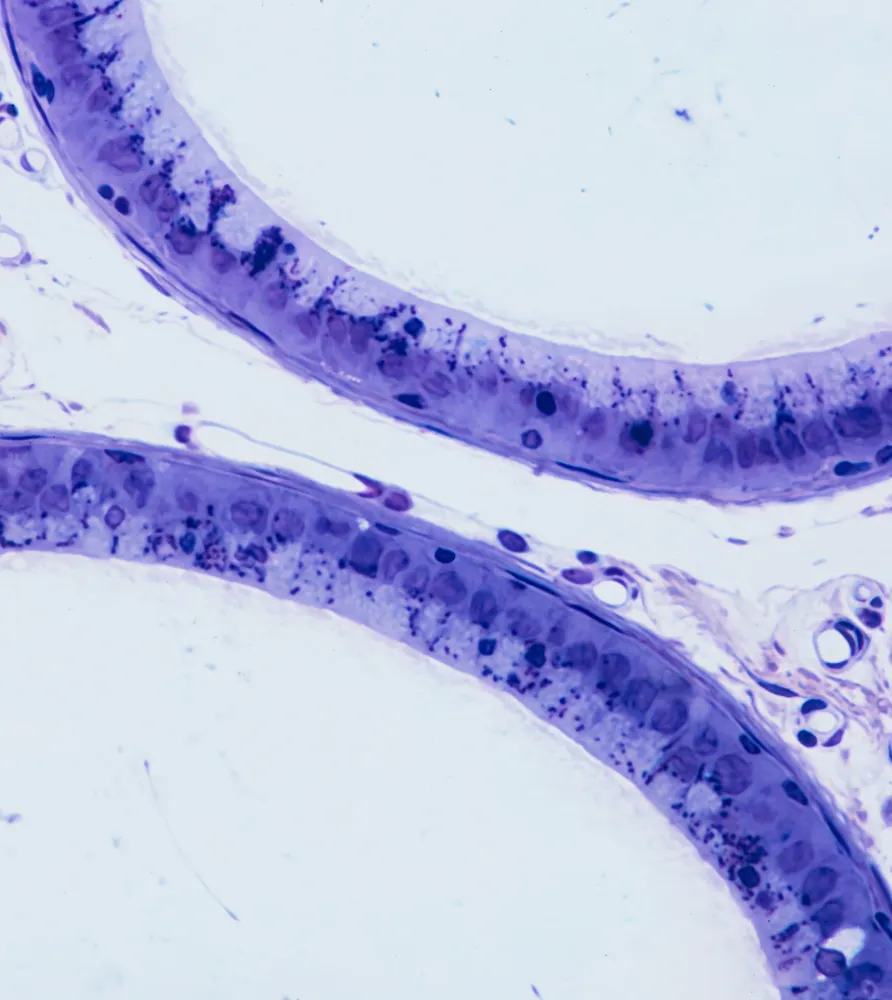
The epididymis is a tightly coiled, crescent-shaped duct located on the back of each testicle that collects, stores, and matures sperm made in the seminiferous tubules of the testes. As sperm travel through the 20-foot-long (when uncoiled) epididymal tube, they gain motility and the ability to fertilize an egg.
When the epididymis becomes blocked or scarred, sperm cannot reach the vas deferens—the tube that carries them out of the body—resulting in low sperm count or azoospermia (zero sperm in the ejaculate). In some men, the obstruction affects only one side, lowering sperm count; in others, it occurs on both sides, causing complete infertility.
What Causes an Epididymal Blockage?
Epididymal obstruction can occur for a variety of reasons, including:
Infection
The epididymis is the most infection-prone structure within the scrotum. In younger men, infections often arise from sexually transmitted infections (STIs), while in older men they are more likely to result from urinary or bacterial infections. When untreated, inflammation can lead to scarring and permanent blockage.
Prior Surgeries or Scrotal Procedures
Past hydrocele or spermatocele repairs, hernia surgeries, or procedures for testicular torsion can unintentionally damage or scar the epididymal duct, blocking sperm flow. Even procedures meant to prevent torsion (orchidopexy) may occasionally cause obstruction.
Vasectomy-Related Pressure
Men who have undergone a vasectomy, especially a traditional “closed-ended” one, may develop pressure buildup behind the closure point. This can cause the fragile epididymal tubules to rupture and scar down over time—a condition sometimes discovered years later during a vasectomy reversal consultation.
Trauma or Injury
Direct trauma to the scrotum—during childhood, sports, or accidents—can also lead to epididymal scarring and blockage.
Diagnosing Epididymal Obstruction
Diagnosis begins with a comprehensive urological evaluation. During a physical exam, Dr. Werner may feel that the epididymis is enlarged, firm, or hardened—a key sign of obstruction, since a normal epididymis feels soft and flat.

Additional diagnostic tests may include:
- Semen analysis: to detect low or absent sperm count.
- Hormone testing: to confirm normal sperm production.
- Scrotal ultrasound: to visualize structural abnormalities or dilation.
- Testicular biopsy: if needed, to confirm that sperm production is normal within the testes.
If the testicles are producing sperm but none are found in the ejaculate, the diagnosis points toward epididymal or ductal obstruction rather than a production problem.
Treatment Options for Epididymal Obstruction
Fortunately, epididymal obstruction is highly treatable. The goal is either to restore natural sperm flow or retrieve viable sperm for use in assisted reproduction.
1. Microsurgical Reconstruction (Vasoepididymostomy)
When feasible, Dr. Werner performs a vasoepididymostomy, a delicate microsurgical procedure that bypasses the blockage by directly connecting the vas deferens to a healthy segment of the epididymis.
- This procedure re-establishes sperm flow into the ejaculate, potentially allowing for natural conception.
- Success rates depend on the location of the obstruction and the surgeon’s microsurgical expertise—Maze’s experience in male fertility microsurgery makes these outcomes highly favorable.
2. Sperm Retrieval Techniques
If surgical repair is not possible or desired, Maze offers advanced sperm retrieval options:
- Microsurgical Epididymal Sperm Aspiration (MESA): Sperm are collected directly from the epididymis under a microscope. MESA is ideal because sperm retrieved here are more mature and more numerous than those obtained from the testis, improving success rates in IVF with ICSI (intracytoplasmic sperm injection).
- Testicular Biopsy or Needle Aspiration: For patients where MESA is not suitable, sperm can be extracted directly from the testis. These procedures are minimally invasive and performed under local or light anesthesia.
- Retrieved sperm are then frozen (cryopreserved) for future use, often providing enough material for multiple IVF cycles.
3. IVF/ICSI
In cases where sperm are retrieved but not naturally ejaculated, Maze collaborates with IVF specialists to fertilize eggs through in vitro fertilization (IVF) combined with ICSI, in which a single sperm is injected into each egg.
Your Next Steps at Maze Men’s Health
If you’ve been diagnosed with an epididymal obstruction or have been told you have azoospermia, you are not out of options. The majority of men with this condition can achieve pregnancy—either naturally or through assisted reproductive technologies—when guided by an experienced male infertility specialist.
At Maze, every patient receives a personalized fertility roadmap—combining diagnostic precision, cutting-edge microsurgery, and compassionate care. Whether your goal is to restore sperm flow or retrieve viable sperm for IVF, we’ll help you understand every step and make informed, confident decisions.
About Dr. Werner and Maze

About Dr. Werner
About Maze
















Maze facility
Areas served
Patient Stories
Our deepest thanks for your support in our fertility journey
We want to express our deepest thanks for your support in our fertility journey.
We are still very much in the throes of our family building story, but as we reflect back on the last year, the moment we stepped into your office is one of our biggest turning points. We were terrified, and your guidance, reassurance, and compassion during a time of extreme uncertainty for us meant more than words can express. That moment when you let us know that having biological children would be a possibility for us will hold a special place in our hearts for the rest of our lives.
Your ability to create an atmosphere of comfort and understanding sets a benchmark in patient care that is truly unparalleled.
L, NY
I deeply appreciate the efforts you and your staff have made...
Maze has created an experience of gaining insight and comfort with and acceptance of, my post surgical sexual self.
Based on my experience with Maze, I would highly recommend you, your clinicians and staff, to others — your approach and quality of concern and support (and determination!) have been hugely valuable.
A, NJ
I have been a patient for almost 10 years...
If you want to go to an office where everyone there is encouraging, helpful, and sincere then Dr. Werner and staff is the place for you. I have been a patient for almost 10 years and never did I think it was about money for his operation.
They have always gave me clear information and guided me through any procedure or process I was working through. I would recommend this office to anyone that needs help!
SR, NY, 49
I could not recommend Dr. Werner and his great team more highly!
I have been seeing Dr. Werner and his fine staff for a few years now and simply put-its the best medical care I’ve ever experienced. Due in large part to the guidance and healthcare I’ve experienced here I feel like the best version of myself at age 41. I could not recommend this Dr. Werner and his great team more highly! Thank you all for what you do!!
JC, NY, Age 41
I Wish I Could Give Them More Stars!!
This is an amazing place!!!! Not only is Dr. Werner great, but the entire staff is incredible. They have completely changed my life for the better. Only wish I had known about them sooner. I wish I could give more stars!!!
David, NY, Age 39
I am in great, knowledgeable, and experienced hands.
Excellent care and follow up by Dr. Werner and Nick. As a doctor myself, I feel I am in great, knowledgeable, and experienced hands. A+
A, NY, Age 44
To state that Dr. Werner saved my life, would be an understatement!
I have been under his care for almost a decade during which he guided me through successful Peyronies treatment, a penile fracture, erectile dysfunction, and in the end, a life beyond my wildest dreams. Dr. Werner, Nick, Paul, Rima, and his entire staff, have spent so much time investing in my physical health, in an effort to not only solve medical problems, but to maximize my overall quality of life.
Dr. Werner is beyond a great practitioner. He’s a great man. His balance of exemplary knowledge, comprehensive treatment, humor, and individualized patient care, has far exceeded any expectation that I have ever had for a doctor. This is to say that Dr. Werner has always treated me as a human being, first. Therefore, his understanding of the person whom he treats, in addition to only the most sound scientific research, makes his work life-altering.
Over the past 10 years, I have continually peppered his staff with questions and concerns, as I have always felt the need to stay educated. Backed by tremendous patience and humility, Dr. Werner has never made me feel like a number. I feel grateful that I found his office, years ago. To that end, I no longer consider him, Nick, or Paul, mere practitioners, but dear friends. I owe much, if not all of my progress over the last few years, to MAZE MENS HEALTH.
Alix B, NJ, Age 51
Dr. Werner and team are knowledgeable, confident and really care about you as an individual!
My first impressions of Dr. Werner: smart, caring, confident, warm. He really listened to me and demonstrated a high level of confidence that he could help me. He understood the impact my symptoms were having on my life and didn’t minimize them. Paul (therapist) and Kristy (exercise physiologist) were also professional and inspired both calm and confidence.
I was initially referred to Dr. Werner for ED and began using a combination of medication and penile injections. Once Dr. Werner found the right dose for me, I was able to get the best erection I had had in over six months. I later developed Peyronie’s Disease as well. I was fortunate that Dr. Werner had significant experience treating Peyronie’s Disease, as he was able to assess me and recommend Xiaflex injections. While treating my Peyronie’s, Dr. Werner also suggested I begin Shockwave Therapy to further help my ED. Since completing both treatments, not only has my Peyronie’s seen dramatic improvement, but my ability to get an erection has improved 95%!
I feel very positive about my experience with Dr. Werner and Maze. These are good people and they are good at what they do. They understand the problem, treat you with respect and take your concerns seriously. I can’t imagine there’s any sexual health issue Dr. Werner would not be able to help you with! If you do consider coming to Maze, it’s important to stick with it and remember that these are medical issues and results do not happen overnight. I was incredibly nervous when I came in for my first appointment, but Dr. Werner has created an environment and a team at Maze that will immediately put you at ease.
Additionally, you and your partner must be on the same page since treatment is a process and requires both patience and good communication. I’m happy to say my wife and I have seen tremendous benefits, becoming even more communicative and closer as a couple throughout this process. Two years ago, I never would have believed coming in for treatment would have changed our relationship so positively.
D, PA, Age 69
Bottom line is that Dr. Werner and all the staff were wonderful!
Very impressive and professional medical practice. Top staff, rigorous process, timely service and excellent follow-up. There is also a positive and vibrant demeanor projected by everyone in the office that I have not seen in other places. There is extensive testing that can get pricey for out of network patients, but cannot argue with the treatment process, quality and results. Bottom line is that Dr. Werner and all the staff are wonderful!
AP, NY, Age 63
The word I would use for Dr. Werner is “thorough."
In 2009, I came to see Dr. Werner for erectile dysfunction, but I was having symptoms for ten years before I got here! I had seen many other urologists, but they just couldn’t figure it out. When I found Dr. Werner, all that changed.
I was very impressed with the caring and knowledge he possesses. He really went out of his way to find out everything that was a piece of my issues. The word I would use for Dr. Werner is “thorough.”
He discovered that I had low testosterone as well as erectile dysfunction. Once I started treatment he had me come in every 4-6 months to check my numbers and regulate me. Together, we found the right treatment cocktail, and my issues were resolved within 4-6 weeks!*
If you ever feel, at any point in your life, that there is a problem, seek help immediately!
A, NY, Age 47
Dr. Werner combines thoroughness with panache.
Dr. Werner combines thoroughness with panache. I feel like his care is totally comprehensive and I feel total confidence that no details will be missed. I have very high standards and he more than surpassed them all.
R, NY, Age 59
Dr. Werner helped us start a family. We will always be extremely thankful.
How are you, Bat Sheva, and Dr. Werner? We hope all of you are doing well and I’m sure helping people move towards sexual wholeness.
We’re doing really well. Our little miracle from God, Anna Joy, is almost 5 months old now!! She is rolling over, babbles a lot, and has the cutest toothless smile. Stan and I absolutely adore her and marvel every day that God gave us this amazing little girl to take care of. We’re so blessed.
We will never forget how Dr. Bat Sheva, and Dr. Werner played such a vital role in our journey towards parenthood. We will always be extremely thankful to God for you.
Please send our love to them.
S & J, NJ
Most compassionate, friendly doctor.
I have been a patient of Dr. Werner’s for over 21 years and he is the most compassionate, friendly doctor I have ever met.
I look for his advice even outside of his specialty. The same can be said for Nick and all of the staff at Maze.
A, NY, Age 59
I followed instructions to rest the first two days and had NO pain.
After many conversations with my girlfriend, I decided to take responsibility for our birth control. As a 46 year old divorced medical professional with 4 children and in a long term committed relationship, this was the right decision. I was scared to death to have a vasectomy and in fact I am even afraid of needles for blood work. I made my appointment because I knew that if I didn’t set it up I wouldn’t go through with it.
I was given an appointment within a few days. The office staff was amazing and the surgical coordinator was so helpful with all of my questions. My consult with Dr. Werner could not have been any better. He is so personable and nice, and put my mind at ease promising that he would adjust the medications for me because he could tell how anxious I was.
I then came back a few days later for my pre screening. As I mentioned I am petrified of blood draws. The phlebotomist and medical tech, Ben, drew my blood and I didn’t even feel it. On the day of the procedure I took the medications as prescribed and barely felt or remember a thing. I followed the instructions to rest the first two days and had NO pain! I can honestly say that I would recommend Dr. Werner and his staff to anyone who is ready to have a vasectomy and take on the responsibility of birth control in their relationship.
MO, Age 46
Dr. Werner and his staff are absolutely the best.
Dr. Werner and his staff are absolutely the best. I have been a patient for 2 years and I actually enjoy my appointments because everyone is so nice and knowledgeable. I had a vasectomy and it was an easy procedure at this office with no pain and a very quick recovery. I have no problem recommending to other men that they get this procedure if they have finished having children.
Maze offers other good quality services, such as counseling, fitness testing, testosterone treatment, and sperm banking.
If you’re hesitant about vasectomy procedures or seeking treatment for male issues, I can say that this office makes you feel comfortable and at ease. Not once did I ever feel awkward. Professional and caring, the way a doctor’s office should be.
BR, NY, Age 52
I am in disbelief that I was symptom free all weekend.
I’m just writing in to thank you for such a seamless, painless, and gratifying vasectomy experience last Friday. I am in disbelief that I was symptom free all weekend and cannot visually see any evidence of the procedure! How is this possible???
R, NYC, Age 48
I felt no pain during or after the procedure!
I went to Maze Men’s Health because I was interested in the needle-less and scalpel-less technique used by Dr. Werner. The staff was great. Very friendly and professional. You felt comfortable and welcome from the moment you stepped inside the office door. Dr. Werner is great. Photos and diagrams were used to thoroughly explain the procedure. And he is an engaging man so you feel he is going to do the best job possible. He treated me as if I were a family friend. The prep for the procedure was quick and the actual operation lasted no more than 20 minutes. During that time Dr. Werner was cracking jokes, we were having a great conversation and the next thing I knew he was finished. I felt no pain during or after the procedure. This is written on day 2 and I have no pain or swelling in the area. I HIGHLY recommend Maze for anyone thinking about a vasectomy or any other services that they provide. Thanks Dr. Werner!!!
A, CT, Age 52
The entire experience was stress-free....and painless.
Before I moved to Westchester, I had decided to undergo a traditional vasectomy but chickened-out at the last minute. Once I moved, I was traveling on the Metro North train and noticed an ad for the no-needle, no-scalpel vasectomy at Maze Men’s Health. I immediately called to find out more information.
From the moment I met Dr. Werner, he made me feel completely at ease in what could potentially have been a very high anxiety situation. Although I was worried about the pain, there was absolutely no pain at all!
I couldn’t believe how easy the process was. From the first call through follow-up after the procedure, the entire experience was stress-free. I would definitely recommend Dr. Werner to anyone considering a vasectomy.
V, NY, Age 43
Dr. Werner and the entire Maze staff was FANTASTIC.
My experience with Dr. Werner and the entire Maze staff was fantastic. From the front desk, to billing, to the clinical staff and right up to Dr. Werner himself, my experience has been excellent. From consultation, pre-op, procedure and post visits everyone has been tremendously professional and great to work with. Today I’m 1000% healed up and extremely happy I came to see Dr. Werner in the first place.
M, NY, Age 38
Frequently Asked Questions
How long does the no-scalpel vasectomy take?
About 20 minutes; most patients say the recovery is easier than a dental procedure.
When can I drive?
Same day if you only used nitrous (no oral meds). If you took oral meds, arrange a driver.
Is the incision visible?
It’s a tiny opening—no stitches—and often hard to find afterward.
Is it reversible?
Reversal is possible but not guaranteed. Consider this permanent; some patients bank sperm before.
Will insurance cover it?
Many plans reimburse most or all costs. Our team handles claims and pre-authorization.
